
ECHO-Chicago: Urinary Incontinence in Primary Care-Summer 2022
Non-surgical treatment, including behavioral interventions or pharmacotherapy, is usually effective, but recognition in health care settings and evidence-based care for this condition remains suboptimal. In fact, only half of the estimated 40% of Medicare beneficiaries with UI who have spoken to a physician receive treatment. Treatment in primary care, with system support and availability of specialty care, has great potential. Unfortunately, a variety of patient, provider, and system-level barriers result in under-diagnosis and suboptimal management.
ECHO-Chicago in partnership with UI specialists and primary care physicians from University Hospitals Cleveland Medical Center Urology Institute has put together this series to increase the workforce capacity of nurse navigators and primary care physicians who are working with medically complex individuals with urinary incontinence. Funding from AHRQ will support planning and implementation of the UI series. The series is comprised of eight one hour-long sessions that will be facilitated by a team of subject matter experts. Sessions will consist of short didactic presentations (~20-30 minutes), followed by participant-led case presentations (new and follow-up cases). This structure, modeled after medical rounds, allows participants to apply the knowledge gained and openly discuss the real-world challenges of implementing recommended best practices. Through these discussions, the series facilitators and participants draw on their own experience to support each other and share strategies that they have found to be successful in navigating barriers.
The goal of this activity is to increase the workforce capacity of nurse navigators and primary care physicians working with medically complex individuals with urinary incontinence.
Target Audience
Learning Objectives
At the conclusion of this activity, participants will be able to:
- Define urinary incontinence (UI), its causes, types and prevalence;
- Describe the basic office evaluation of UI;
- Discuss how to manage UI using behavioral therapy like bladder diary and bladder training;
- Define third-line overactive bladder (OAB) treatment, its indications and contraindications, and treatment options;
- State how physical therapy can be used to manage UI;
- Identify advanced management techniques for OAB, including onabotulinumtoxinA, percutaneous tibial nerve stimulation, and neural stimulation therapy;
- Name surgical management techniques for stress UI, including bulking and slings;
- Recognize a complex patient that is a good candidate for early referral.
- 8.00 AMA PRA Category 1 Credit™
- 8.00 Participation
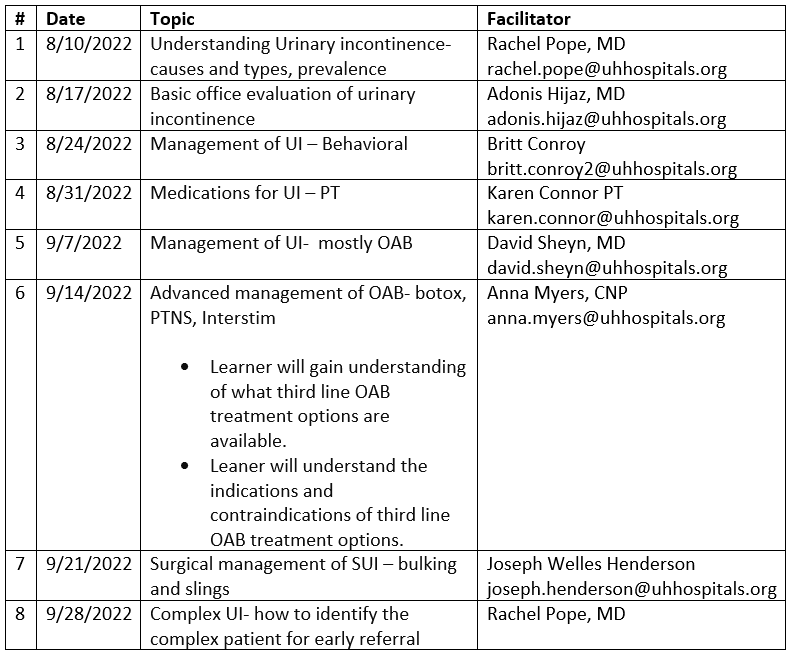
Agenda subject to change.
WANT TO KNOW MORE?
ACCESSIBILITY The University of Chicago is committed to providing equal access appropriate to need and circumstances and complies fully with legal requirements of the Americans with Disabilities Act. If you are in need of special accommodation, please contact ECHO-Chicago via e-mail via at [email protected].
The University of Chicago reserves the right to cancel or postpone this conference due to unforeseen circumstances. In the unlikely event this activity must be cancelled or postponed, the registration fee will be refunded; however, The University of Chicago is not responsible for any related costs, charges, or expenses to participants, including fees assessed by airline/travel/lodging agencies.
COURSE DIRECTOR
Disclosure Declarations
As a provider accredited by the ACCME, The University of Chicago Pritzker School of Medicine asks everyone in a position to control the content of an education activity to disclose all financial relationships with any ineligible companies. This includes any entity whose primary business is producing, marketing, selling, re-selling, or distributing healthcare products used by or on patients. Financial relationships are relevant if a financial relationship, in any amount, exists between the person in control of content and an ineligible company during the past 24 months, and the content of the education is related to the products of an ineligible company with whom the person has a financial relationship. Mechanisms are in place to identify and mitigate any relevant financial relationships prior to the start of the activity.
Additionally, The University of Chicago Pritzker School of Medicine requires Authors to identify investigational products or off-label uses of products regulated by the US Food and Drug Administration at first mention and where appropriate in the content.
The University of Chicago Pritzker School of Medicine is accredited by the Accreditation Council for Continuing Medical Education (ACCME) to provide continuing medical education for physicians.
The University of Chicago Pritzker School of Medicine designates this live activity for a maximum of 8 AMA PRA Category 1 Credits™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Other healthcare professionals will receive a Certificate of Participation. For information on the applicability and acceptance of Certificates of Participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by the ACCME, please consult your professional licensing board.
Claiming Credit: Enter the access code to unlock the credit claiming process.
Please Note: The credit claiming process will close three months after the conference end date. Requests to claim credit after three months will be subject to additional fees.

 Facebook
Facebook X
X LinkedIn
LinkedIn Forward
Forward